Mission
The mission of the Quality and Patient Safety (QPS) division of the Department of Anesthesiology is to provide the highest level of care to patients in a safe environment. To achieve this goal, we support individual anesthesia clinicians at NewYork-Presbyterian/Weill Cornell Medical Center as they provide safe and reliable clinical care.
We hold Quality and Patient Safety (QPS) education programs for residents and fellows, and collaborate with national quality improvement and patient safety networks.
Quality and Patient Safety Curriculum
Goals
- Foster a culture of safety to ensure a secure and professional work environment for anesthesiology residents.
- Educate on key principles of quality improvement methodologies and support efforts to enhance patient and family care.
- Share quality improvement and patient safety indicators relevant to anesthesiology practice to increase awareness of individual and departmental performance compared to national standards.
Objectives
Upon completing the Department of Anesthesiology’s Quality Improvement and Patient Safety Residency Curriculum residents will be able to:
- Identify patient safety concerns and opportunities for improvement within healthcare systems.
- Understand the adverse event reporting and review processes utilized by the Department of Anesthesiology and NewYork-Presbyterian Hospital.
- Apply quality improvement (QI) methods and collaborate in interdisciplinary teams to enhance the efficiency and effectiveness of patient care systems.
- Recognize challenges and barriers associated with performance improvement initiatives.
- Understand anesthesiology-related quality improvement and patient safety indicators, and how to improve individual clinical practice to meet departmental and national standards.
Quality Improvement (QI) Education Day
This full-day course is designed to introduce and teach participants the tools and methodology they need to conduct a successful quality improvement initiative. Residents and fellows tackle quality initiatives through a workshop led by NYP Clinical Systems Engineers. The workshop walks participants through the steps involved in completing such a project, including defining the problem, assessing the root cause, and brainstorming success measures. This provides them with the framework to address problems that arise in healthcare systems with the ultimate goal of enabling physicians to improve patient safety and quality of care.

Resident-Driven QI Program
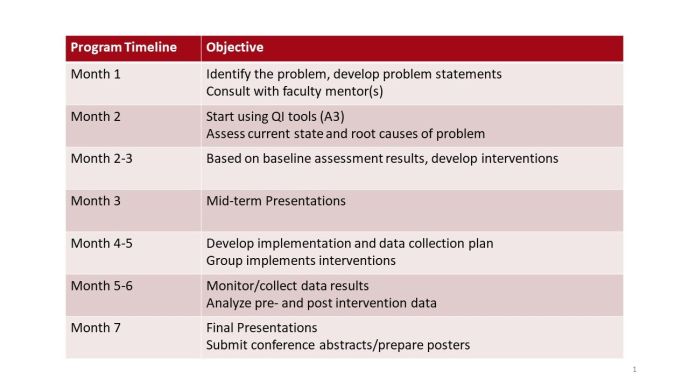
The Resident-Driven Quality Improvement (RDQI) Project program provides our residents with formal training on QI methodology, practical project experience, and the opportunity to collaborate with interdisciplinary teams across NewYork-Presbyterian Hospital (NYPH). This multifaceted program equips our physicians with the knowledge to improve the efficiency and effectiveness of patient care systems by appropriately identifying challenges and barriers in the evolving healthcare environment.
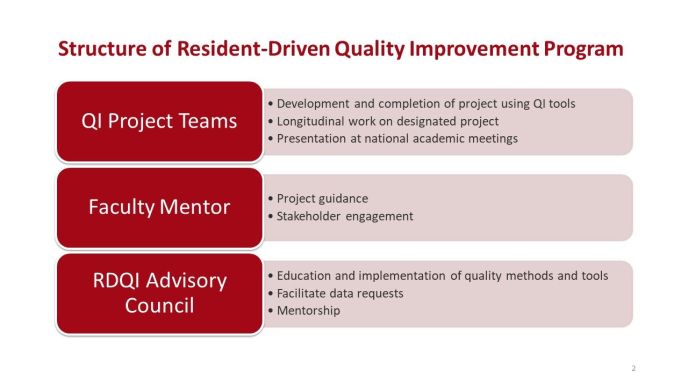
Residents kick off the program by undergoing a full-day training at QI Education Day led by the department and NYPH Clinical Systems Engineers to learn the foundation and essentials of QI methodology. The learnings are then applied in their year-long QI project initiatives to streamline and improve clinical practice within the department and hospital. Throughout the year, they are guided by a faculty mentor and the RDQI advisory council, comprised of the QPS chair, QPS administrator and QPS coordinator.
Residents have gone on to present their project successes at Grand Rounds and in local and regional conferences, including the New York Academy of Medicine, PostGraduate Assembly in Anesthesiology, and American Society of Anesthesiologists.
Root Cause Analysis (RCA) Observation
Root Cause Analysis (RCA) is a systematic approach to identifying and understanding the causes of an identified problem. By identifying these system flaws, we can correct each appropriately to prevent the error from happening again, rather than focusing on blame. Residents have the opportunity to attend and observe RCA meetings throughout the year. A structured debrief is then held directly after the meeting to solidify understanding and clarify any questions the residents may have.
Quality Improvement Initiatives
QPS Committee Overview
The QPS Committee reviews all patient care events and presents their findings at monthly meetings. They discuss quality improvement strategies and use a departmental dashboard to monitor and analyze trends in anesthesia care events.
Anesthesiology Patient Safety Award
The Anesthesiology Patient Safety Award, instituted by the QPS Committee, serves as a key initiative to foster a culture of safety within the department. This prestigious award is presented to a clinician who has demonstrated exceptional commitment to promoting patient safety and enhancing the quality of care. Recipients are honored during the departmental Grand Rounds, where they receive the award along with a small gift card as a token of appreciation for their invaluable contributions.
Anesthesia Performance Improvement Reporting Exchange (ASPIRE)
ASPIRE is a quality improvement initiative comprised of over 40 hospitals across the nation focused on decreasing variation in care in processes known to impact postoperative complications and cost. Anesthesiologists receive individualized feedback regarding their performance on various patient safety indicators.
For more information, please visit: https://mpog.org/aspire/
Patient Safety Awareness Week
In celebration of National Patient Safety Awareness Week, the Department of Anesthesiology annually organizes a series of luncheons and breakfasts across local campuses. These events bring together anesthesiologists, residents, CRNAs and staff to engage in meaningful discussions about departmental patient safety initiatives. Attendees explore innovative strategies to enhance patient safety and elevate the quality of care. Additionally, the program includes educational training sessions designed to provide valuable insights and practical skills for improving patient outcomes.
Who We Are

Patricia Mack, MD
Vice Chair for Patient Safety & Quality Improvement
Associate Professor of Clinical Anesthesiology









